&me Anti Stigma Campaign
A campaign to encourage senior, currently well healthcare professionals including doctors, vets, dentists and pharmacists to informally self identify as having experienced a mental health condition in order to reduce the stigma of mental health in the healthcare professions.


Our inspiring &me volunteers
List of services
-
Vet Kirstie Pickles
Vet Kirstie Pickles frankly discusses her experience of anxiety and depression as well as her recent diagnosis of autism. 'I am very open about being autistic, both to help myself stay well and reduce my triggers and also to encourage other people that it is ok.'
-
Vet James Glass
Vet James Glass was diagnosed with severe depressive disorder in 2018 and was off work for nine months. James writes: 'Life is absolutely worth living again and, while I might not have chosen this pathway, it’s a privilege to use my experience to help others.'
-
Vet Ebony Escalona
'The manic highs can often be part of great things such as founding Vets Stay Go Diversify. They remind me that I’m beautifully human and I’m not a robot and that big mental health moments have acted as important pivot points for me to reevaluate what I want to do and why. Be them in the phases of my hypomania or my depression.'
-
Dr Serena Haywood, consultant paediatrician
On the aftermath of a traumatic work experience:
'The fear and isolation of this event led me to take the risky decision to start talking about my mental health as much as I could to as many people as would listen. I was advised not to but did it anyway. And my life changed from there. '
-
Caroline Elton, occupational psychologist & author of 'Also Human'List Item 1
'I don’t want to collude with the fantasy that depression, or any other mental illness, only happens to other people. It has certainly happened to me.'
-
Vet Nurse Meghan Conroy
'My mental health is a part of me, but it does not define me. Certainly not as a nurse.'
-
Vet Allisdhair McNaull
'It was at this time I realised that I needed help. It had only taken me 25 years to come to this realisation.'
-
Dr Becky Hirst, consultant palliative medicineList Item 2
'I wouldn’t wish the experience on anyone, but I could not have gained such insights into the world and myself without it. Depression leaves a stain on your soul, even when you fully recover, but that scar serves to remind me of the journey I’ve made and be grateful.'
-
Vet Stephanie WalshList Item 3
'Hopefully by sharing my story, we can work to reduce the stigma, and open early channels of communication to help look after the mental health of ourselves and others.'
-
Dr Rebecca Lawrence, consultant psychiatristList Item 4
'Adapt if you need to because of the illness, but never because of the stigma of the illness, whether self-stigma or otherwise.'
-
Vet Steve Carter
'The single most important realisation for me was that I am always going to be vulnerable and it was necessary to come to terms with that “weakness” whether I liked the idea or not.'
-
Dr Cathy Wield, emergency medicine doctor
Cathy is passionate about speaking out and reducing the stigma around mental health.
'There is still a long way to go to eliminate not only the stigma of current mental illness, but also of the past. While I worked in A&E until August last year, I did my utmost to be open about myself and to educate my colleagues.'
-
Prof. Jamie Hacker Hughes, psychologist
Jamie says that it is really important that people at the top of the profession speak openly about the fact that they are human too!
-
Vet Rob Pettitt
'We would not hesitate to tell people if we broke a bone; the same should apply to mental health.
What surprised me was the number of people who have been affected and you will always find someone who has been there – support from others is invaluable in those difficult times so you do not have to suffer alone.'
-
Dr Susan Atcheson, general practitioner
'Stigma can be addressed and challenged but this work needs recognition, involvement and reinforcement. We all have to take part.
For my part "My name is Susan, I am a senior GP and I have a history of depression".'
-
Dr Malcolm Kinnear, consultant psychiatrist
Malcolm finds that having taken some of the medications he now prescribes can be rather helpful in terms of understanding their effects!
-
Dr Caroline Walker, psychiatrist & psychotherapist
'The worst stigma I've experienced over the years was the stigma I put on myself.
Speaking out about my illness has helped me to feel less ashamed - I now feel incredibly proud of my experiences and the way I manage my mental health.'
-
Dr Angelika Luehrs, consultant psychiatrist
'When I asked for advice about how to access help one of the answers I got was one of ‘whatever you do, make sure that you don't have any mental illness in your medical records otherwise you will never go anywhere in your medical career'.
However, getting the diagnosis (bipolar affective disorder) and help from a Consultant Psychiatrist was the best thing that ever happened.'
-
Vet David Bartram
'My episode of mental ill-health by no means defines me but it’s an important part of me and, although I would not wish it upon anyone, I think it has changed me in a positive way, both personally and professionally.'
-
Dr Jonathan Richardson, consultant psychiatrist & medical director
'It is 24 years since my mental illness. I now work in Northumberland, Tyne and Wear NHS Foundation Trust, one of the largest mental health and learning disability trusts in England – and one of only two to be rated outstanding by the Care Quality Commission…. I do not feel that my illness has stopped me.'
-
Dr Louise Freeman
'When I was sick, I was told that a colleague had ‘always thought that I was a mental health problem waiting to happen.’
On reflection, yes that was true, but only in as much as this applies to ALL of us during our lives.'
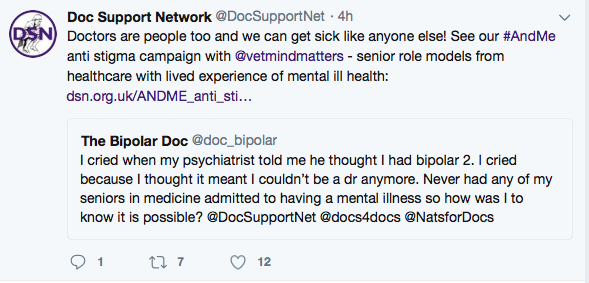
Author and psychiatrist Dr Linda Gask speaking about &me and her recent Guardian column

&me launch at House of Commons Tuesday 31st January 2017







&me Anti Stigma Campaign Outline
- Northumberland, Tyne and Wear NHS Foundation Trust – NTW is a major mental health trust in the North of England. Chief executive John Lawlor is open about his own history of depression. The trust has recently been involved in the ‘Time to Talk’ campaign from ‘Time to Change’.
- Royal College of Psychiatrists – previously ran the ‘Changing Minds’ campaign and its president Professor Sir Simon Wessely is particularly interested in stigma.

